
The Definitive Guide To Reversing Fatty Liver - Part 2
Do you know what causes fatty liver? You may be surprised to learn it is not usually caused by eating too much fat. Also, it is not just overweight people who can get a fatty liver. It can actually be caused by a number of factors. The more you know about fatty liver, the better equipped you will be to reverse it and restore your health.
Causes of Fatty Liver
If you have a fatty liver, it may have been caused by one or more of these factors:
- Incorrect diet – ingesting excess carbohydrates and processed food high in polyunsaturated processed vegetable oils.
- Insulin resistance. This means eating more carbohydrate than your body can tolerate and results in excess blood levels of insulin (called hyperinsulinemia)
- Excess body weight, especially around the torso (although it can occur in slim people who have a very poor diet)
- Type two diabetes
- Malnutrition causing deficiencies in protein and vitamins
- Exposure to very toxic substances
- Chronic viral infections
- Excess alcohol intake. This varies among people. Those with a leaky gut cannot tolerate as much alcohol and are more at risk of liver damage from small to moderate amounts of alcohol.
- Some medications can cause fatty liver if they are taken for a long-time including pain killers, corticosteroids, antipsychotic medications, statins, and tamoxifen.
Fatty liver can be associated with polycystic ovarian syndrome in women and low thyroid conditions and unhealthy gut bacteria (dysbiosis) and sleep apnea. These things need to be treated to improve fatty liver.
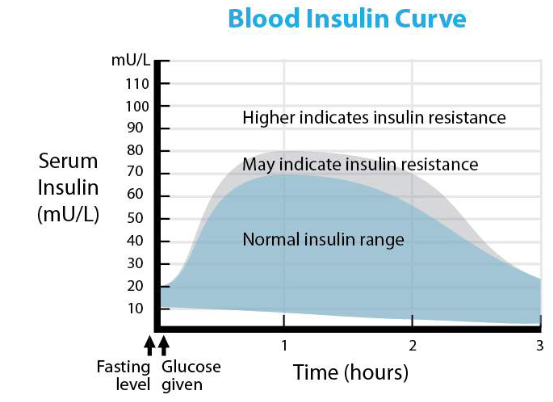
More about insulin resistance
Insulin resistance that may lead to type 2 diabetes can cause fatty liver. In insulin resistance the insulin levels are too high because the insulin does not work efficiently and does not allow the body to burn carbohydrate for energy – instead, carbohydrate gets turned into fat. Insulin is a fat storing hormone.
Insulin resistance is also known by the names Metabolic Associated Fatty Liver Disease (MAFLD), Syndrome X or Metabolic Syndrome. It can cause inability to lose weight, elevated blood pressure and fluid retention.
Metabolic Associated Fatty Liver Disease is really a problem with how the metabolism handles dietary carbohydrates. Many patients with MAFLD develop cardiovascular disease or cancer but they can also develop severe liver disease.
There is NO approved medication treatment for MAFLD and nutritional medicine and lifestyle modification has been proven to work well. A study of 293 patients showed an improvement in liver fibrosis in 90% of patients who achieved weight loss of more than 10%.
It is also important to avoid medications that can cause fatty liver such as corticosteroids, valproic acid, methotrexate, and amiodarone.
Note: When abnormal liver function tests are discovered, it is important to exclude other types and causes of liver disease
Fatty liver is often overlooked
Many people have a liver which is too fatty or overburdened by toxic chemicals; but what I see all the time is that they don’t realise this is the reason their health is down, and they are not getting better. Some doctors underestimate the liver’s role in failure to recover from illness or achieve good health. Doctors are trained to treat liver disease but often by then it’s too late. It is not safe to just monitor the progress of an unhealthy liver when there are safe reliable ways to reverse liver inflammation.
Recently I saw a middle-aged man who was struggling to get over long COVID because it had given him blood clots. I explained to him that because he had a fatty liver, he would not achieve his pre-COVID health status. However, he could reverse his problem by improving his liver by quitting sugar, eating more vegetables, good quality protein and drinking more water and freshly made juices from lime, lemon, and grapefruit. He would also need to take Livatone Plus which is a world leading clinically tested liver formula.
How is fatty liver disease diagnosed?
Fatty liver often has no symptoms, or only vague symptoms, so your doctor may be the first one to spot it.
Higher levels of liver enzymes (elevated liver enzymes) or elevated serum ferritin (iron) levels that turn up on a blood test for other conditions, or on a routine annual blood test check, should raise a red flag for fatty liver.
Elevated liver enzymes and/or ferritin are a sign your liver is injured.
To confirm a diagnosis of fatty liver your doctor may order the following tests -
- Tests to image the shape, size and texture of your liver – namely Ultrasound scan or Computed Tomography (CT scan)of the abdomen.
- Liver biopsy(tissue sample) to determine how far the liver disease has progressed.
- FibroScan – a fibroscan is a specialized ultrasound scan sometimes used instead of a liver biopsy to find out the amount of scar tissue in the liver. Fibrosis in the liver can be detected and is classified as stage F1 to F4, with F4 being more severe (cirrhosis). Fibrosis severity is a predictor of more risk of severe liver disease. A fibroscan is a non-invasive test and is safer than a liver biopsy.
Long term follow-up of fatty liver
The progression of fatty liver disease can vary but in patients who develop fibrosis, regular monitoring is essential to avoid liver cancer and cirrhosis. Ideally the liver should be checked annually, but in patients with stage 2 cirrhosis, pre-cirrhosis, or cirrhosis, it is wise to consult a liver specialist. They should be checked every 6 months for liver cancer with a liver ultrasound scan and blood tests for the cancer marker alfa-fetoprotein.
Early to medium stages of cirrhosis can be reversed with nutritional medicine.
Fatty Liver – it can be reversed
If you focus on improving your liver health, you can see enormous benefits within a few months. Your liver responds beautifully to some TLC. This is not surprising because your liver is the most strategic organ for overall health in your body. Studies have shown that fatty liver disease can be reversed with nutritional medicine, and the earlier the better. I have written a book titled FATTY LIVER YOU CAN REVERSE IT
See part 3 next week for a FREE eating guide on how to reverse fatty liver.
Reference
Reference: AJGP. Volume 50, Issue 10, October 2021
Updates in fatty liver disease: Pathophysiology, diagnosis and management
doi: 10.31128/AJGP-05-21-5974
The above statements have not been evaluated by the FDA and are not intended to diagnose, treat or cure any disease.
Know someone who might benefit from this article? Share it!
4 Comments
Need Help?
1-888-75-LIVER
Monday to Friday, 9:00 am to 5:00 pm MST
100%
Satisfaction Guaranteed
If it’s faulty or wrongly described, we’ll replace it.











We are pleased you have eliminated both the HCV and HBV from your liver although we expect there may still be some residual damage.
Having Type 2 Diabetes will further retard your ability to have your liver at best possible function because most diabetics have Fatty Liver.
Insulin resistance is your body’s response to blood glucose being too high on a regular basis.
This is expected when the diet is high in processed foods, foods high in carbohydrates, and/or industrial seed oils.
We recommend a liver friendly, anti-inflammatory diet and lifestyle as is found with Dr Cabot’s 15 Day Cleanse and Maintenance Program.
Supplements make the necessary changes far easier so begin taking Berberine 1 to 2 capsules twice daily with meals and Glicemic Balance 1 to 2 capsules 10 to 15 minutes before each meal.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
I take livatone plus. I would like to know your views on tudca , as dr Eric Borg talks a lot about this on reversing fatty liver. It has been found in mice to decrease insulin levels, and to decrease fatty liver. I currently take duloxettine (Cymbalta) for anxiety. Can I take tudca safety ? I have asked my dr but she doesn't know .
Sonia
Sydney Australia
Dr Cabot does not carry a TUDCA product and she has a strong belief in the value of Ox Bile and its value in helping with liver disease and we recommend a dose of 1 to 2 capsules twice daily during meals.
In addition to Livatone Plus we recommend you begin NAC – 2 capsules twice daily with a large glass of water to avoid temporary stomach irritation.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD