

When The Stomach Does Not Work: Gastroparesis
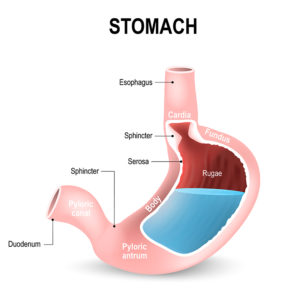
The term gastro means stomach and the word paresis means partial paralysis – so gastroparesis means partial paralysis of the stomach. Gastroparesis affects around 4% of the population. In gastroparesis the movement of the stomach muscles has become weakened or impaired. This weakness is most commonly due to damage to the nerves that supply the stomach.
The vagus nerve controls the muscles and secretions of the stomach, small intestine, gall bladder and pancreas.
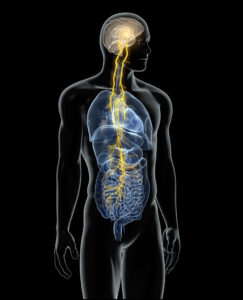
The vagus nerve starts in the brain and travels a long way down through the chest and abdomen to supply the esophagus and stomach muscles. The vagus nerve tells the stomach muscles when and how much to contract. Anything that damages the vagus nerve can cause gastroparesis as well as many other problems.
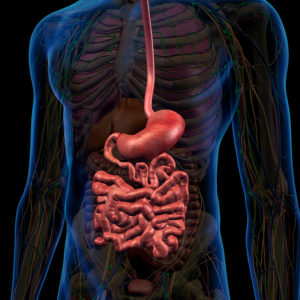
Your stomach is the first part of the intestines to receive the food you eat and swallow. The muscles in your stomach must contract strongly to move the food along and empty the stomach. If the stomach muscles don’t work properly the food stays in the stomach and the stomach swells to a larger size. This is called delayed gastric emptying.
What are the causes of gastroparesis?
- Diabetes is the most common cause of gastroparesis. This is because diabetes damages nerves, and in this case, it is the vagus nerve that gets damaged by the high blood sugar levels. The high blood sugar levels also damage special cells, called pacemaker cells, in the wall of the stomach. These pacemaker cells control the rhythm of the stomach muscle contractions.
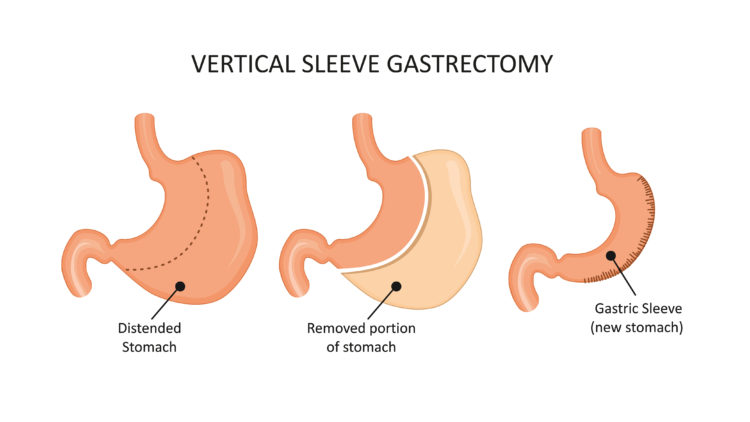
- Surgery on the upper gastrointestinal tract (esophagus, stomach, or small intestine), may damage the vagus nerve. Weight loss surgery known as bariatric surgery (sleeve gastrectomy or gastric bypass) can damage the vagus nerve causing gastroparesis in a small percentage of patients. However, paradoxically it was found by some surgeons that sleeve gastrectomy relieved gastroparesis in patients with severe symptoms.
- Some cancer treatments, such as radiation therapy to the stomach area and some types of strong chemotherapy can damage the vagus nerve.
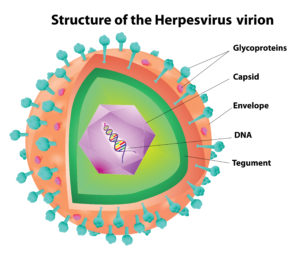
- The herpes virus can get into the vagus nerve causing severe damage to the nerve. This is often not diagnosed correctly, and treatment is therefore incorrect or not given at all.
- Other causes of dysfunction of the vagus nerve and stomach muscles include magnesium deficiency, eating disorders, and opioid drugs.
- Less common causes of gastroparesis include autoimmune connective tissue diseases such as scleroderma and neurological conditions such as Parkinson’s disease.
In around 30% of cases, the cause of gastroparesis is unknown.
What are the symptoms and consequences of gastroparesis?
People with gastroparesis can experience many unpleasant symptoms including feeling too full from small amounts of food, bloating, nausea, vomiting, reduced appetite, abdominal pain, burping and gas, reflux and heartburn and regurgitation of food. This can result in weight loss and severe nutrient deficiencies. There can be an overgrowth of bacteria in the small intestines which can lead to night sweats and aches and pains.
Blood sugar levels can become more unstable, especially in diabetics with phases of low blood sugar while food remains in the stomach, and high blood sugar when food eventually reaches the small intestines.
Some people can develop intestinal obstruction caused by masses of solid hardened food known as bezoars.
Tests for Gastroparesis
It is best to see a specialist in the gut called a gastroenterologist as gastroparesis can be confused with other gut disorders and needs an accurate diagnosis.
The specialist may order the following tests:
- Gastric emptying scans
- An upper gastrointestinal series called a barium swallow Xray.
- Gastroscopy
- Abdominal ultrasound scan
- Gastric or duodenal manometry
Treatment of gastroparesis
The treatment depends upon the cause.
Diabetics need to control their blood sugar levels and in type two diabetes this is best done with getting into the healthy weight range and a low carbohydrate diet. Try avoiding all grains, processed foods and sugar and you may get a big improvement. We have an excellent book on reversing Diabetes Type Two.
A good supplement to stabilize blood sugar levels is called Glicemic Balance and one capsule can be taken with every meal.
Meals need to be small and more frequent as large meals are not tolerated. It is also best not to drink fluids with meals.
If you have trouble with high fiber vegetables, you can make a raw juice out of them with a juice extracting machine.
Cold and hot vegetable soups and bone broth can have high nutritional value and are easy to digest.
Protein requirements: Scrambled eggs can provide a complete source of protein. A smoothie made with coconut cream, whey protein powder, water, a raw egg, and a fruit such as banana, berries, mango or papaya can boost protein intake and is easy to digest. Taking a Digestive Enzymes supplement should help meals to be digested more thoroughly. This reduces overgrowth of yeast and bacteria in the gut, which can feast on undigested food.
Drink plenty of water in between meals.
Keep your intake of alcohol low and avoid artificial sweeteners such as aspartame and sucralose. Artificial sweeteners can damage nerves.
Magnesium supplements can make a big improvement and I recommend Magnesium Ultrapotent Powder in a dose of half a teaspoon twice daily in water.
If you suspect that the herpes virus may have damaged your vagus nerve, I highly recommend you take the supplement called Selenomune to inactivate the virus. This will also reduce inflammation in the vagus nerve. Damage to the vagus nerve from the herpes virus is more likely in people who have had cold sores or shingles in the past.
Exercise to help the solar plexus and the vagus nerve such as Pilates or Yoga and stretching. Gargling and gagging also stimulate the vagus nerve.
Medications
Medications can help to alleviate symptoms and include:
Motility drugs to increase the speed of intestinal contractions (peristalsis); these may help the stomach to empty quicker. Motility drugs include metoclopramide and domperidone. In severe cases a drug called cisapride can be prescribed but must be monitored for possible side effects.
Antiemetics to reduce nausea and vomiting; these include medicines such as prochlorperazine, promethazine and ondansetron. Ondansetron can be every effective to relieve nausea and vomiting and is a safe drug.
Surgery
A gastric electric stimulator is an implanted device that provides controlled electrical pulses to stimulate the muscles in the stomach to speed up gastric emptying. This treatment is not always successful and is not available in all areas.
Botox (botulism toxin) injections into the sphincter that connects the stomach to the small intestine can relax the sphincter muscle so that it more easily allows food passage from the stomach into the small intestine. Botox injections are not always successful and can become less effective with repeat injections.
Sleeve Gastrectomy
Surgeons from The Center for Metabolic and Weight Loss Surgery suspected that a laparoscopic procedure called sleeve gastrectomy, normally used for rapid weight loss, could help patients with severe gastroparesis. A study from the Cleveland Clinic showed that gastric bypass surgery is effective in morbidly obese gastroparesis patients and safer than subtotal gastrectomy. Consult a surgeon who specializes in gastric surgery if you cannot get relief with more conservative measures.
A feeding tube surgically attached at the entry to the small intestine can be used as a last resort if the patient is unable to eat.
Gastroparesis is a very distressing condition and can destroy your quality of life. By understanding it more and trying the measures described in this article you may get a big improvement, a modest improvement, no improvement or a complete cure. You will not know until you try!
The earlier gastroparesis is diagnosed and corrected, the higher the chance of a successful outcome.
The above statements have not been evaluated by the FDA and are not intended to diagnose, treat or cure any disease.
Know someone who might benefit from this article? Share it!
8 Comments
Need Help?
1-888-75-LIVER
Monday to Friday, 9:00 am to 5:00 pm MST
100%
Satisfaction Guaranteed
If it’s faulty or wrongly described, we’ll replace it.











I took Ozempic, two days only, half dose for weight loss. I from then couldn’t keep food or water in at all and ended up with hospital and was diagnosed with gastroperesis. I thought this was my biggest problem but I believe I have been healing this. I was prescribed domperadone and was out on mirtazipan. I lost 20 kilos in 3 months. After I ate only bone broth chicken and vegetable soup I made and a savoury mince vegetable dish.
Since my mental health has been absolutely crazy. Severe anxiety, cyclical thoughts. I have had maybe a couple of days in a year I have felt normal.
I have bloods every 4 weeks and am told they are all very normal. I have noticed I am worse symptom wise with my stomach and head at from 5 days before period and ovulation times. I have maybe 6 days in the cycle I feel normal. Hormones are apparently normal and thyroid. I have endo and (the sister condition can’t remember. Never used to have sore or lumpy breasts and have this now too. Had checked and cysts.
Any suggestions on the mental health component?
It sounds like you've had a very difficult time of it lately.
We hope things will get better for you.
You may find this article helpful:https://www.liverdoctor.com/poor-liver-health-may-mean-poor-mental-health/
Kind regards,
Jessah Shaw
Nutritionist
Please check out Dr Cabot’s recent videos on the gallbladder, especially this onehttps://www.liverdoctor.com/gallbladder-series-part-7-gallbladder-surgery/
Also, please check out her video on gastroparesis:https://www.liverdoctor.com/gastroparesis-causes-symptoms-treatment-diet-exercises/
Many people with Gallbladder problems, still have a congested liver remaining after surgery and this is best reversed to improve your general health by reducing inflammation. The most common cause of gastric reflux is low stomach acid and the most common reason for gallbladder removal is liver congestion.
Now that you no longer have a gallbladder it is important to ensure there is sufficient bile present at each meal.
To supply bile, boost liver health and your vitality, Dr Cabot prescribes
Ox Bile capsules – 1 – 2 capsules during each meal to replace the bile that can no longer be delivered from your gallbladder to help essential fat and fat-soluble vitamin absorption.
Livatone Plus – Start with 1 capsule twice daily for the first 2 weeks and then increase to 2 caps twice daily, to improve liver function.
N-Acetyl-Cysteine (NAC 600mg) – Start with 1 cap twice daily for the first 2 weeks and then increase to 2 caps twice daily well away from food, if any upset occurs take at the beginning of your meals. This supplement works well with Livatone Plus to get your liver better faster. This supplement is the precursor nutrient of glutathione; the body’s strongest anti-oxidant. NAC should be taken with a whole glass of water away from food. Do not take just before retiring to bed. NAC can be strong on the stomach, and this is why you need to take it with a whole glass of water.
These can be purchased herehttps://www.liverdoctor.com/products/supplements.html
Kind regards,
Jessah Shaw
Nutritionist
If bile is the wrong consistency (which is what I think you mean), this means it is too high in cholesterol and toxins, and too low in bile salts and this can cause gallstones.
If you watch my videos on gallbladder you will learn about the best diet and supplements. Diet is super important! Perhaps you eat lots of processed foods, carbs and sugar?
If you do not have severe symptoms, you can save your gallbladder.
Start taking Livatone Plus capsules to get your liver making healthier bile. NAC is most helpful to dissolve sludge and stones but needs to be taken in between meals with a large glass of water
Best wishes
Dr Sandra Cabot
www.liverdoctor.com
I use Ox Bile and Berberine HCI, and digestive enzymes to help. I didn't like the prescription stuff or how it made me feel!
Love you and Christine!
We're so happy that you have found relief in our supplements.
Please let us know if you have any further queries.
Kind regards,
Jessah
Nutritionist