
Hemochromatosis
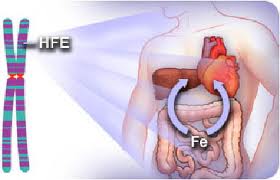 Hemochromatosis is a disorder of iron regulation – it is an inherited disease where excess "free" iron is deposited in various organs including the liver, heart, joints and pancreas. The iron is 'free' because it is not bound tightly to carrier proteins which would otherwise prevent it from damaging cells.
Hemochromatosis is a disorder of iron regulation – it is an inherited disease where excess "free" iron is deposited in various organs including the liver, heart, joints and pancreas. The iron is 'free' because it is not bound tightly to carrier proteins which would otherwise prevent it from damaging cells.
The iron cannot be broken down and eliminated from the body and this leads to iron overload in the body. The iron accumulates over a long period of time and early diagnosis is vital as the excess iron is stored gradually over a lifetime. The earlier it is diagnosed, the less chance of development of liver cirrhosis, liver cancer, heart disease and diabetes.
The condition occurs more commonly in men – this is due to the fact that women have regular monthly blood and thus iron loss due to menstruation.
Hemochromatosis is often a silent disorder that is commonly picked up in younger persons during routine blood tests for other problems. However, as iron slowly accumulates in the organs over the years, other complaints may arise such as arthritis, liver problems, heart problems and diabetes.
The presence of this excess iron creates toxic free radicals that damage cells and tissues leading to liver damage (cirrhosis), pancreatic damage (diabetes), heart problems and joint problems. After many years, the risk of liver cancer is high
How do you get this disease?
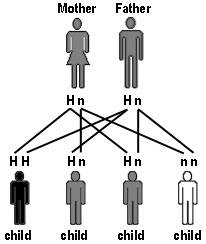 Hemochromatosis is an inherited condition. The disease may be passed on when 2 people who are carriers of the gene for the condition have a child. There is then a one in four chance that this child may have an active form of the disease. The parents and any unaffected children are carriers of only one gene and will not generally develop problems related to excess storage of iron.
Hemochromatosis is an inherited condition. The disease may be passed on when 2 people who are carriers of the gene for the condition have a child. There is then a one in four chance that this child may have an active form of the disease. The parents and any unaffected children are carriers of only one gene and will not generally develop problems related to excess storage of iron.
Who should be tested for this condition?
If you have been diagnosed with hemochromatosis it is wise to have your blood relatives screened – and your spouse if you plan to have children. It is found in people of Northern European descent and is most common in the Irish.
Orthodox treatment
Treatment of hemochromatosis consists of regular venesections (removal of blood, similar to a blood donation). Venesection, if done regularly, will prevent the disease completely, provided it is started early enough in the person's life; thus the importance of early diagnosis. However, it is never too late to start venesections. Treatment is life long.
What are the symptoms of hemochromatosis?
- There may be no symptoms
- Persistent fatigue
- Abdominal discomfort
- Swollen liver/raised liver enzymes
- Joint pains
- Bronzed colouration to the skin
- Elevated blood sugar levels
The triad of bronze skin, enlarged liver and diabetes mellitus is only present in cases of very severe iron overload.
Tests
The test used to diagnose hemochromatosis is the HFE gene analysis for C282Y mutation. This requires a blood sample.
Diet
- Follow the principles of eating in "The Liver Cleansing Diet" book and make these principles a way of life.
- Minimize the intake of foods which are especially high in iron – these include the offal meats - such as liver, heart and kidney, and foods prepared from these such as pate, liverwurst and haggis. Also avoid black pudding - which is made from pig's blood.
- Avoid foods fortified with iron - Many breakfast cereals are fortified with iron, so read the ingredients list on the pack.
- Avoid supplements or tonics containing iron.
- Use caution with alcohol - the recommended level is a maximum of 4 - 5 standard drinks a week.
For curry lovers it is advisable to avoid 'balti' curries cooked in traditional cast iron pots. These meals can contain more iron than the most iron-rich foods such as liver. - NOTE - You do NOT have to avoid vitamin C supplements or foods high in vitamin C - this is a common myth and will be bad for your health if you are low in vitamin C. You do NOT have to avoid red meat as it has health benefits and provided you are having regular venesections these foods containing iron will not harm you.
General recommendations
- Make sure you have your iron levels checked every 3 months.
Recommended books
- "The Liver Cleansing Diet". Follow the principles for a healthy liver outlined in this book. This book is essential reading for anyone with liver dysfunction and contains sections on fatty liver, liver function tests, hemochromatosis and high cholesterol, etc. These principles of eating need to be followed as a way of life.
- “Raw Juices Can Save your Life”
Raw juicing
Juices are vitally important as a source of powerful antioxidants. It is good to use both whole fruits and vegetables in the diet as well as the juices, as the juices provide an easily absorbed form of nutra-ceuticals that are beneficial for the liver. Lots of useful and delicious recipes can be found in “Raw Juices Can Save your Life” book.
Recommended supplements for hemochromatosis
- Livatone Plus Capsules
Take 1 teaspoon stirred in water or juice twice daily, or take 2 capsules twice daily. A combination of St Mary's Thistle, NAC, vitamins and taurine and natural antioxidants play a vital role in promoting a more vigorous liver detoxification required after toxic overload. - N-Acetyl-Cysteine (NAC) 600mg capsules take one to two capsules twice daily
The above statements have not been evaluated by the FDA and are not intended to diagnose, treat or cure any disease.
Know someone who might benefit from this article? Share it!
18 Comments
Need Help?
1-888-75-LIVER
Monday to Friday, 9:00 am to 5:00 pm MST
100%
Satisfaction Guaranteed
If it’s faulty or wrongly described, we’ll replace it.











My mom died of iron overload (hemochromatosis) she was told she was just a carrier. The lack of knowledge most doctors have results in damage to the body before you can get the help you need to avoid it. She passed away as a result. I am also a carrier and was told by my doctors that because I was a carrier I have just a 3% chance of getting it. The lack of preventive phlebotomy ( because even now my levels are in normal range. ( mid to high side of normal) I had heart failure from my pregnancy with my twins 19 years ago, I am diabetic, I have now this week been told I have cirrhosis of the liver although last year in the hospital ( form a severe auto immune response form the covid vaccine) I was told my liver is normal. MY two children have both genes, one from my husband and one from me. So at this point I am trying to do what I can to not get worst. I have a liver doctor appointment tomorrow and I do go to a naturopathic dr as well. I wasn't to try and reverse some of this so I have been doing a lot of research alternate day fasting seems to help the liver. when my mom was still alive I bought her Sandras book which she ignored. What can I do to aggressively take action to heal and reverse some of this before tits too late. I will fast, juice fast, do what ever it takes. Because I do feel natural solutions in the past have helped me the most. I also have thyroid disease. Hashimoto's. I need to find out how to eat long term to make it better and what supplements will be most helpful because there is so much conflicting info on the internet.
Hashimotos thyroiditis is common and caused by autoimmune antibodies (TPO markers). To protect your thyroid from more damage you need to get the antibodies down.
The main thing to avoid is grains = wheat, rye, barley, oats and also avoid processed junk food and fast food.
Try to avoid sugar except fruit. You can get nice chocolate sweetened with stevia which is healthy and tasty.
Please check out Dr Cabot’s book ‘YOUR THYROID PROBLEMS SOLVED’.
Please check out Dr Cabot’s recent videos on cirrhosis here:https://www.liverdoctor.com/hepatitis-what-is-it-causes-of-hepatitis-cirrhosis-hepatitis-treatment/
We recommend a number of remedies to ensure your liver is restored to best possible health.
We are delighted to let you know that Dr Cabot has a 15 Day Cleanse – Two weeks to begin your journey toward improved overall health and function, utilising both supplements and a tasty, easy to prepare dietary regimen. Please go tohttp://www.drcabotcleanse.com to place an order.
After completing the Cleanse, we recommend you remain on this style of eating and you can then begin the Maintenance plan that is available at the same website.
To boost liver health and your vitality, Dr Cabot prescribes
Livatone Plus – 1 cap twice daily for 2 weeks and then increase to 2 capsules twice daily, to improve liver function.
N-Acetyl-Cysteine (NAC 600mg) – 1 cap twice daily for 2 weeks and then increase to 2 capsules twice daily well away from food, if any upset occurs take at the beginning of your meals. NAC should be taken with a whole glass of water away from food. Do not take just before retiring to bed. NAC can be strong on the stomach, and this is why you need to take it with a whole glass of water. This supplement works well with Livatone Plus to get your liver better faster. This supplement is the precursor nutrient of glutathione; the body’s strongest anti-oxidant (You will need to call us on 02 4655 4666 to order this, as it is practitioner-only).
Collagen Food – Take 1 teaspoon daily. MSM is a source of organic sulphur, which assists phase 2 liver detoxification and also helps to reduce the formation of scar tissue.
These can be purchased here:https://www.liverdoctor.com/products/supplements.html
Kind regards,
Jessah Shaw
Nutritionist
I just purchased your Livatone Plus supplements, and noticed it has a
really high level of Vitamin B-12 (60 mcg/2500% RDA) - I have Hereditary HEMOCHROMATOSIS and noticed your Hemochromatosis article recommended using Livatone Plus. I've also heard that Vitamin B-12 should be avoided if you have Hemochromatosis because it can raise iron levels even further. Any truth to that? Just wanted to confirm before I start taking them! (Is there ANYTHING in the Livatone Plus supplement that isn't safe if I have Hereditary Hemochromatosis?)
THANK YOU!
The genes that represent hemochromatosis vary in the degree that they affect your ability to remove iron from the body, which gene is represented in your family?
Vitamin B12 at 60mcg is not a high dose and will not affect your hemochromatosis status, and Dr Cabot said it will not raise your iron levels higher.
Avoiding meat and Vitamin C will not make your condition worse and Dr Cabot suggests you have a phlebotomy every three months or as needed to keep your iron, iron saturation, and ferritin levels within normal range.
Diet is very important to keep your liver as healthy as possible because iron overload is very inflammatory. We recommend you begin Dr Cabot’s 15 Day Cleanse and Maintenance Program.
Suitable supplementation is Livatone Plus, NAC, and Fish Oil.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
It is most unusual for iron supplements inducing ferritin excess unless you do have genetically determined hemochromatosis.
Many people have elevated ferritin due to a congested or Fatty Liver and it is most important to also determine if your circulating iron is also elevated.
Only if both are elevated, you can have a phlebotomy to remove a considerable amount of blood to lower all iron levels to a more normal level quickly.
For best liver health Dr Cabot prescribes Livatone Plus.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
Thank you for your enquiry.
Even though there is iron in these seeds, the level is not high and the iron in plants is not very well absorbed so it is unlikely to contribute much to any iron overload concerns.
3½ oz of flaxseed contains 5.73mgs of iron, 3½ oz of oats contains 4.7mgs of iron and we were not able to find a reputable source for iron in chia seed. It is far more likely that you would consume 3½ oz or more of oats but we would not expect you to eat more than ½ to 1 oz of flaxseed, so the amount of iron in your breakfast is not significantly increased.
It is important to ensure that you still have sufficient protein daily, and it is also important to have a regular source of Vitamin C, so we recommend that you do not have vitamin c rich foods within 2 hours of eating foods that contain iron.
Liver health is especially important for those with hemochromatosis to have their liver is as vibrant health as is possible and Dr Cabot prescribes
Livatone Plus – 1 to 2 capsules twice daily, to improve liver function.https://www.liverdoctor.com/livatone-plus.html
N-Acetyl-Cysteine (NAC 600mg) – 1 to 2 capsules twice daily well away from food, if any upset occurs take at the beginning of your meals. This supplement works well with Livatone Plus to get your liver better faster. This supplement is the precursor nutrient of glutathione; the body’s strongest anti-oxidant and potent detoxifier.https://www.liverdoctor.com/nac-n-acetyl-l-cysteine-600mg-90-capsules.html
MSM + Vitamin C – ½ to 1 teaspoon twice daily in vegetable juice or water to reduce oxidation, inflammation and boost liver health.https://www.liverdoctor.com/msm-plus-vitamin-c-powder-100-grams.html, but ensure this is taken well away from any foods containing iron.
You may purchase these supplements and Dr Cabot’s books athttps://shop.liverdoctor.com/
Was hemochromatosis diagnosed by a gene test or because your ferritin test result was very high?
Kind regards
Victoria Taylor
Naturopath
The article states to minimize the intake of foods which are especially high in iron – these include the offal meats - such as liver, heart and kidney, and foods prepared from these such as pate, liverwurst and haggis. It then says you do NOT have to avoid red meat. I hope this clarifies things for you.
Kind regards,
Jessah Shaw
Nutritionist for Liverdoctor.com
Cow's milk is a good source of protein, calcium and B vitamins.
Coconut milk is a good nondairy option and contains medium-chain triglycerides (MCTs) which researchers have linked with weight loss.
It is not very high in iron as 100 g of coconut milk only contains 1.6 mg of iron.
Kind regards,
Jessah Shaw
Nutritionist for Liverdoctor.com
That amount of vitamin C is safe for people with high ferritin.
Kind Regards,
Jessah Robinson
Nutritionist for Liverdoctor.com
It would be better to avoid all cow's milk and instead use almond, rice or coconut milk instead.
Kind Regards,
Jessah Robinson
Nutrition Consultant for Liverdoctor.com
Is it OK to take organic sulfur crystals if you have hemochromatosis?
Many thanks
There should be no issues taking organic sulfur crystals.
Kind Regards,
Jessah Robinson
Nutrition Consultant for Liverdoctor.com