
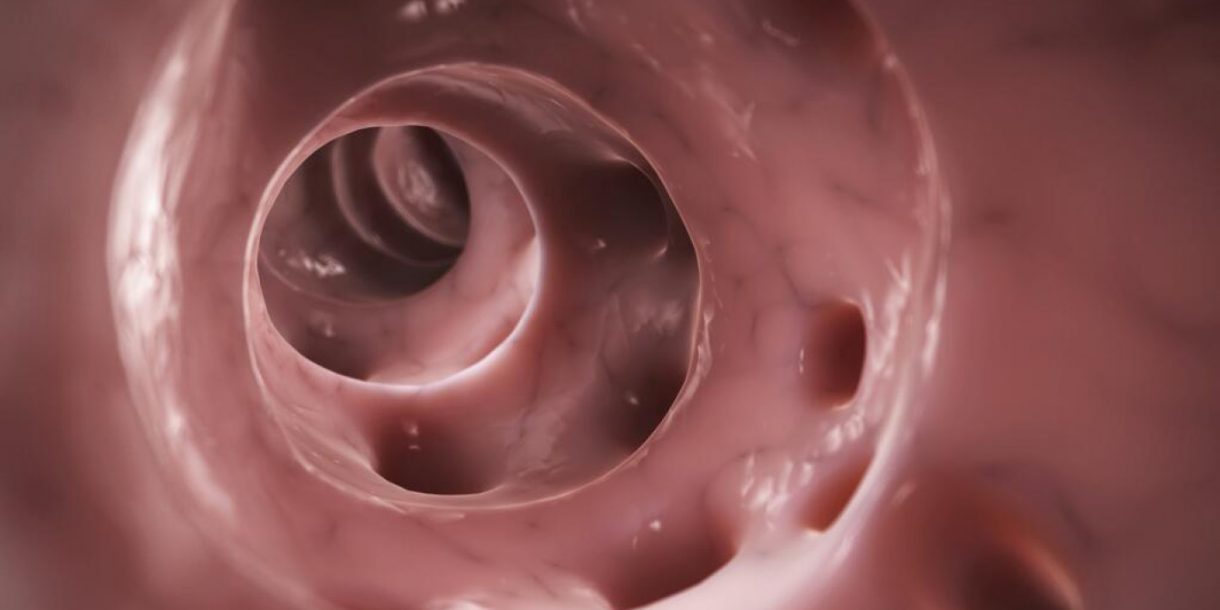
What Really Causes Diverticulitis?
Diverticulitis is incredibly common, yet the most common dietary advice given to patients may be incorrect.
Diverticula are small pouches that bulge outward through the large intestine (colon). If you have these pouches, you have diverticulosis. Diverticulosis becomes increasingly common as people age. It is estimated that half of all people over age 60 have it.
Most people with diverticulosis don't have any symptoms. Occasionally they may experience mild cramps, bloating or constipation. Diverticulosis is often discovered while a person is undergoing tests for something else. Many people first discover they have diverticula pockets in their bowel while they are undergoing a colonoscopy screening for colon cancer.
If the pouches become inflamed or infected, this is referred to as diverticulitis. Abdominal pain is the most common symptom, and it’s usually on the left size. Depending on the severity, some people also experience fever, nausea, vomiting and constipation. In very severe cases, diverticulitis can cause tears in the bowel that bleed, or blockages in the bowel.
Conventional treatment usually consists of antibiotics, pain relievers, and a temporary liquid diet. Occasionally surgery is deemed necessary.
What causes diverticulitis? What foods should be avoided?
If you have been diagnosed with this condition, your doctor has probably told you to avoid eating nuts and seeds. Is that really the best advice? A study published in the Journal of the American Medical Association titled “Nut, corn and popcorn consumption and the incidence of diverticular disease” found no evidence at all to support this recommendation.
The study followed more than 47,000 people who were aged between 40 and 75 years, for 18 years. Not only did this research fail to find a direct link between eating nuts, seeds and popcorn and bouts of diverticulitis, it actually found the precise opposite.
The more nuts, seeds and popcorn a person eats, the less likely they are to ever develop diverticulitis.
The study concluded with the statement that “The recommendation to avoid these foods to prevent diverticular complications should be reconsidered.” You can read the entire study here.
So what causes diverticulitis?
A long history of constipation and straining is the biggest risk factor for developing diverticulosis. Dry, hard stools and fecal impaction also increase the risk because they raise pressure in the intestines and the muscles of the colon have to work harder to try and push the fecal matter along.
Irritable bowel syndrome and gluten intolerance are also risk factors. Basically having a history of digestive problems raises your risk of developing diverticula pockets in your colon as you get older. If those pockets become infected with bacteria, or if feces becomes trapped in them, diverticulitis develops and this can progress to a medical emergency.
Recommendations for preventing and managing diverticulitis
- It is extremely important to have regular bowel motions which consist of soft stools. If the stool is hard, this will worsen the pockets and raise the risk of infection. Make sure you drink between 8 and 10 glasses of water each day, or herbal tea. The tannins in regular tea can worsen constipation. Make sure you eat some fruit or vegetables at each meal. Prunes, nuts and seeds are also an excellent source of fiber. Make sure you chew them well and do not eat them during a flare up of diverticulitis. If you still struggle with hard stools, the gentle fiber in Fibretone should help. You can add 2 tablespoons to a smoothie, cereal, porridge, muffins, or just stir it into water or vegetable juice.
- If you have a history of irritable bowel syndrome, reflux, heartburn, bloating or gas, you are probably best off avoiding gluten. People with gluten intolerance or celiac disease who continue to eat gluten have an increased risk of diverticulitis. I have found that avoiding gluten offers the vast majority of my patients with diverticulitis significant symptom relief and it reduces the risk of flare ups. There is also some research to show that the insoluble fiber in wheat and other grains raises the risk of diverticulitis in everyone; not just people with gluten sensitivity.
- Make sure there is a good balance between the good and bad bugs in your intestines. An overgrowth of harmful gut bacteria or fungi is incredibly common. It is very important to avoid developing a bowel infection, as this can lead to a medical emergency. Sugar and yeast can encourage the growth of bad bowel bugs. Eating fermented foods like sauerkraut, and consuming garlic and onion helps to keep bad bugs at bay. Intestinal Parasite Cleanse capsules are a powerful formula for keeping your insides clean.
- Taking a probiotic (good bowel bacteria) supplement, and/or eating fermented vegetables is also extremely beneficial.
- If you have an inflamed gut, a glutamine supplement should help to reduce the inflammation and assist tissue healing. Glutamine is used as fuel by the cells lining our intestines (called enterocytes). It can help to keep your gut lining healthy and can offer symptom relief for individuals with diverticulitis. Glutamine can be found in my Ultimate Gut Health powder.
- If you continue to experience digestive problems, you may have an intolerance to one or more foods. It can be difficult to detect the problematic foods, therefore it is best to see a naturopath or nutritionist.
Diverticulitis is a complicated condition, with several causes and aggravating factors. Hopefully these ideas will offer you some help.
The above statements have not been evaluated by the FDA and are not intended to diagnose, treat or cure any disease.
Know someone who might benefit from this article? Share it!
34 Comments
Need Help?
1-888-75-LIVER
Monday to Friday, 9:00 am to 5:00 pm MST
100%
Satisfaction Guaranteed
If it’s faulty or wrongly described, we’ll replace it.











Thank you for reaching out.
We recommend downloading Dr Cabot’s free e-book on gut health here:https://www.liverdoctor.com/ultimate-gut-health-book-free-download/
You would also benefit from following the recommendations in Dr Cabot's book: 'Healthy Bowel, healthy body':https://shop.cabothealth.com.au/healthy-bowel-healthy-body
Best supplement for diverticulitis is BACTOCLEAR one capsule in middle of every meal
Also take NAC Capsules to kill biofilm of chronic infection – take 2 capsules twice day in between meals with a whole large glass of water.
Selenomune Designer Energy – 1 capsule daily to shrink the polyps and boost your immune system to inhibit the processes if your polyps are precancerous.
It is important to have ultrasound scan after 6 months of taking SELENOMUNE to see how much polyps have shrunk.
Kind regards,
Jessah Shaw
Nutritionist
You may find this article helpful:https://www.liverdoctor.com/natural-tips-to-help-diverticulitis/
We recommend downloading Dr Cabot's free e-book on gut health here:https://www.liverdoctor.com/ultimate-gut-health-book-free-download/
Kind regards,
Jessah Shaw
Nutritionist
It certainly does sound like dairy is an issue for you, and as chocolate contains milk, it makes sense that you had symptoms afterwards.
We recommend downloading our free e-book on gut health:https://www.liverdoctor.com/ultimate-gut-health-book-free-download/
You would benefit from taking 'Intestinal Para-clean' and 'Ultimate Gut Health'.
You may benefit from trying our 15 day Cleanse:https://www.liverdoctor.com/15-day-cleanse.html
Kind regards,
Jessah
If your father has Crohn's Disease I advise you to avoid eating gluten. To reduce the unhealthy bacteria in your colon that infect the diverticular pouches in your colon I highly recommend the natural antimicrobial called BACTOCLEAR - take one capsule twice daily in the middle of meals. Drink a lot of water. Raw vegetable juices are also good. Take my ULTIMATE GUT HEALTH POWDER one teaspoon twice day in a glass of water in between meals. See my free e-book titled ULTIMATE GUT HEALTH
Best wishes
Dr Sandra Cabot
Sorry to hear that.
You may find these articles helpful:
https://www.liverdoctor.com/natural-remedies-to-help-you-feel-less-stressed/
https://www.liverdoctor.com/natural-tips-to-help-diverticulitis/
Kind regards,
Jessah Shaw
Nutritionist
You may have a diseased section of colon - get an opinion from a specialist bowel surgeon.
Dairy should not be too bad, sugar and bread is worse.
Best supplement for diverticulitis is BACTOCLEAR one capsule in middle of every meal
Also take NAC Capsules to kill biofilm of chronic infection - take 2 capsules twice day in between meals with a whole large glass of water.
SELENOMUME one capsule day to strengthen immune system
Regards
Dr Sandra Cabot
www.liverdoctor.com
My mother was coeliac as is one of my daughters. I had noticed that when I used to visit my mother and ate the same gluten free diet as her I felt much better, but when I came back home and returned to my gluten containing diet I would have a flare up. Even though I tested negative for Coeliac disease I decided to try going gluten free and have never looked back. I wish I had gone gluten free years earlier. I haven’t had antibiotics for 5 years now and my flare ups are far less frequent and less severe.
We're so glad you have begun to feel better.
Unfortunately there are a lot of doctors who don't know the importance diet can make in many circumstances.
Please let us know if you have any further queries.
Kind regards,
Jessah Shaw
Nutritionst
whole grains can flare up bowel inflammation
there is a big connection between the brain and the gut
MAGNESIUM ULTRAPOTENT POWDER one tsp daily in water helps constipation a lot
you need to read my excellent free e book ULTIMATE GUT HEALTH which covers everything
have a feces test for MCS, and PCR - YOU MAY HAVE PARASITES which need treating
Let me know how you get on
Cheers
Dr Sandra Cabot
Rather than looking at grains other than wheat, rye, barley, and most oats which all contain gluten it may be other dietary items that are irritating your digestive tract and causing over activity of your bowel.
You may have lectin intolerance or FODMAP sensitivity.
As well as the dietary changes that may be required, please begin taking Ultimate Gut Health 1 scoop both in the morning and just before bed each night.
Hardening of the bowel is likely to be due to a magnesium deficiency or because of calcium deposits so begin taking Vitamin K - 1 capsule daily.
Due to your loose tummy it is important to take Magnesium powder or tablets in small divided doses to avoid additional tummy loosening.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
We are so pleased you have found this website and its many articles and recipes so valuable. We look forward to your continued support.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
We are devoted to helping people improve their health and recommend you to search our extensive article library for answers as well as speaking to your primary health practitioner whenever you have health concerns.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
When IBS and diverticular disease is present it is very important to ensure you follow an anti-inflammatory diet and lifestyle and we recommend Dr Cabot’s 15 Day Cleanse and Maintenance Program.
This style of diet is anticipated to normalize your intestinal concerns and reduce the occurrence of any bouts of diverticulitis.
This eating style encourages the growth of beneficial gut bacteria.
To further discourage the growth of non-beneficial microbes Dr Cabot prescribes Berberine, and Ox Bile.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
Thank you for your comments and we completely agree that inflammation is an important contributor to the development of diverticulitis.
Dr Cabot’s book ‘Gluten, Is It Making You Sick or Fat’ addresses your comments and much more.
Once these pouches have developed, they remain for life, and to reduce the potential for flares Dr Cabot’s 15 Day Cleanse and Maintenance Program offers an anti-inflammatory dietary regimen while detoxing the liver, alkalinizing the whole body and healing the digestive tract.
Kind regards
Victoria
Naturopath for Dr Sandra Cabot MD
We are sorry to hear that you are experiencing this.
Bowel issues can be really debilitating.
We recommend following the advise in this article. Hopefully you will find some symptom relief.
Kind regards,
Louise
Increasing fiber isn’t beneficial for everyone. People with irritable bowel syndrome, dysbiosis or small intestinal bacterial overgrowth are more prone to diverticulitis. Stress can make those conditions worse, and so can increasing fiber. Once pockets form, or scar tissue from an abscess, bacterial overgrowth is inevitable. BactoClear capsules may help you, as the herbs in them are a natural disinfectant for the gut.
Kind regards,
Margaret Jasinska
Naturopath for Liverdoctor.com
So glad you noticed an improvement, the water definitely would've made a difference.
Please read our other recommendations in the above article for further improvement.
Kind regards,
Jessah Robinson
Nutritionist for Liverdoctor.com